Tailoring MITRAL VALVE (MV)
Repair with MitraClip™
Results in Unparalleled
MITRAL VALVE REGURGITATION (MR) Reduction

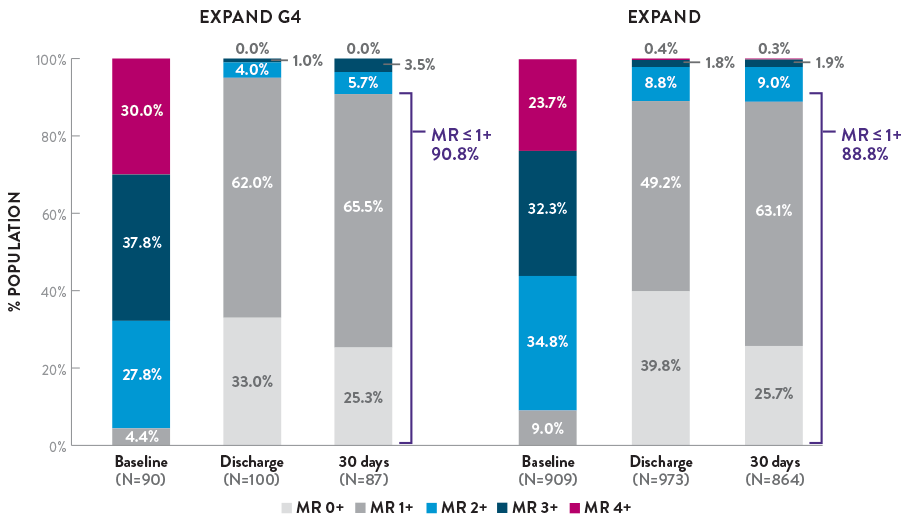
HIGHEST MITRAL REGURGITATION REDUCTION REPORTED TO DATE1
PROVEN MR REDUCTION TO 1+ OR LESS WITH TAILORED REPAIR1
MITRACLIP IS THE ONLY PROVEN Transcatheter mitral
valve (TMV)* THERAPY THAT GIVES YOU CONFIDENCE IN:
SAFETY
96.6% freedom from
device-related complications
at 12 months2
SURVIVAL
• Lowest 30-day and 1 year
mortality rate reported in
large scale real-world studies1
• Only MV device shown to
improve survival in HF patients
with SMR3
DURABILTY
Only TMV device with proven
sustained outcomes to 5 years as
demonstrated by sustained MR
reduction, improvement in heart
failure symptoms, and left
ventricle volumes2-13
EFFECTIVENESS
• 89% ≤ 1+ at 1 year
in PMR and
SMR patients1
• 99% MR ≤ 2+ at 24 months
in SMR patients3
QUALITY OF LIFE
Largest 1-year improvement in quality of life
reported to date1
(Health-related quality of life measured by KCCQ Overall Summary score)
*Transcatheter Mitral Valve
MitraClip has a safety profile supported
by years of clinical use

*Data on file at Abbott.
Primary Safety Endpoint in SMR1
| Primary Safety Endpoint in SMR1 | |
|---|---|
| Total Device-related complications | 9 (3.4%) |
| Single leaflet device attachment | 2 (0.7%) |
| device embolization | 1 (0.3%) |
| Endocarditis requiring surgery | 0 (0.0%) |
| mitral stenosis requiring surgery | 0 (0.0%) |
| Left ventricular assist device implant | 3 (1.2%) |
| heart transplant | 2 (0.8%) |
| Any device-related complication requiring nonelective cv surgery | 1 (0.3%) |
Primary MITRAL REGURGITATION
- Low procedural mortality rate of 6.3% in PMR14
- 19% of patients experienced a major adverse event at 30 days, with transfusion (12.6%) being the most common event, followed by death from any cause (6.3%)15
MAT-2410455 v1.0 | Item approved for U.S. use only
- Rottbauer WD. Contemporary Clinical Outcomes with MitraClip™ (NTR/XTR) System: Core-lab Echo Results from +1000 Patient the Global EXPAND Study. Data presented at PCR 2020.
- Sürder D, Klersy C, Corti R, et al; Collaborators. Impact of mitral regurgitation aetiology on MitraClip outcomes: the MitraSwiss registry. EuroIntervention. 2020;16(2):e112-e120.
- Stone G. COAPT: A Randomized Trial of Transcatheter Mitral Valve Leaflet Approximation in Patients with Heart Failure and Secondary Mitral Regurgitation. Presented at TCT 2018.
- Maisano F. Clip Selection Strategy and Outcomes with MitraClip™ (NTR/XTR): Evidence-Based Recommendations from the Global EXPAND Study. Data presented at PCR 2020.
- Feldman T, Kar S, Elmariah S, Smart SC, et al; EVEREST II Investigators. Randomized comparison of percutaneous repair and surgery for mitral regurgitation: 5-year results of EVEREST II. J Am Coll Cardiol. 2015;66(25):2844-2854.
- Kar S, Feldman T, Qasim A, et al; EVEREST II Investigators. Five-year outcomes of transcatheter reduction of significant mitral regurgitation in high-surgical-risk patients. Heart. 2019;105(21):1622-1628.
- Lim S. Five-Year Durability Results Of Transcatheter Mitral Valve Repair With the MitraClip® System in Patients With Severe Degenerative Mitral Regurgitation and Prohibitive Surgical Risk. Poster presented at ACC 2018.
- Feldman T. The EVEREST II REALISM Continued Access Study: Five-Year Outcomes in High Surgical Risk Patients. Data presented at PCR 2018.
- Feldman T. The EVEREST II REALISM Continued Access Non-High Risk Study: Mid- and Long-Term Follow-up in Surgical Candidates. Data presented at ESC 2017.
- Kalbacher D, Schäfer U, V Bardeleben RS, et al. Long-term outcome, survival and predictors of mortality after MitraClip therapy: results from the German Transcatheter Mitral Valve Interventions (TRAMI) registry. Inter J Cardiol. 2019;277:35-41.
- Adamo M, Grasso C, Capodanno D, et al. Five-year clinical outcomes after percutaneous edge-to-edge mitral valve repair: insights from the multicenter GRASP-IT registry. Am Heart J. 2019;217:32-41.
- Bedogni F, Testa L, Rubbio AP, et al. Real-world safety and efficacy of transcatheter mitral valve repair with MitraClip: thirty-day results from the Italian Society of Interventional Cardiology (GIse) Registry of Transcatheter Treatment of Mitral Valve RegurgitaTiOn (GIOTTO). Cardiovasc Revasc Med. 2020;21(9):1057-1062.
- Buzzatti N, Denti P, Scarfò IS, et al. Mid-term outcomes (up to 5 years) of percutaneous edge-to-edge mitral repair in the real-world according to regurgitation mechanism: a single-center experience. Catheter Cardiovasc Interv. 2019;94(3):427-435.
- Lim Scott D. Contemporary Outcomes with MitraClip™ (NTR/XTR) System in Primary Mitral Regurgitation: Results from the Global EXPAND Study. Data presented at ACC 2020.
- MitraClip™ Clip Delivery System Instructions for Use.
REQUEST AN ABBOTT REP
Rx Only
Important Safety Information
MITRACLIP™ CLIP DELIVERY SYSTEM
- The MitraClip™ G4 System is indicated for the percutaneous reduction of significant symptomatic mitral regurgitation (MR ≥ 3+) due to primary abnormality of the mitral apparatus [degenerative MR] in patients who have been determined to be at prohibitive risk for mitral valve surgery by a heart team, which includes a cardiac surgeon experienced in mitral valve surgery and a cardiologist experienced in mitral valve disease, and in whom existing comorbidities would not preclude the expected benefit from reduction of the mitral regurgitation.
- The MitraClip™ G4 System, when used with maximally tolerated guideline-directed medical therapy (GDMT), is indicated for the treatment of symptomatic, moderate-to-severe or severe secondary (or functional) mitral regurgitation (MR; MR ≥ Grade III per American Society of Echocardiography criteria) in patients with a left ventricular ejection fraction (LVEF) ≥ 20% and ≤ 50%, and a left ventricular end systolic dimension (LVESD) ≤ 70 mm whose symptoms and MR severity persist despite maximally tolerated GDMT as determined by a multidisciplinary heart team experienced in the evaluation and treatment of heart failure and mitral valve disease.
Contraindications
The MitraClip G4 System is contraindicated in patients with the following conditions: Patients who cannot tolerate, including allergy or hypersensitivity to, procedural anticoagulation or post procedural anti-platelet regime; Patients with known hypersensitivity to clip components (nickel / titanium, cobalt, chromium, polyester), or with contrast sensitivity; Active endocarditis of the mitral valve; Rheumatic mitral valve disease; Evidence of intracardiac, inferior vena cava (IVC) or femoral venous thrombus.
Potential Complications and Adverse Events
The following ANTICIPATED EVENTS have been identified as possible complications of the MitraClip G4 procedure: Allergic reactions or hypersensitivity to latex, contrast agent, anaesthesia, device materials (nickel / titanium, cobalt, chromium, polyester), and drug reactions to anticoagulation, or antiplatelet drugs, Vascular access complications which may require transfusion or vessel repair including: wound dehiscence, catheter site reactions, Bleeding (including ecchymosis, oozing, hematoma, hemorrhage, retroperitoneal hemorrhage), Arteriovenous fistula, pseudoaneurysm, aneurysm, dissection, perforation / rupture, vascular occlusion, Emboli (air thrombotic material, implant, device component); Peripheral Nerve Injury; Lymphatic complications; Pericardial complications which may require additional intervention, including: Pericardial effuse on, Cardiac tamponade, Pericarditis; Cardiac complications which may require additional interventions or emergency cardiac surgery, including: Cardiac perforation, Atrial septal defect; Mitral valve complications, which may complicate or prevent later surgical repair, including: Chordal entanglement / rupture, Single Leaflet Device Attachment (SLDA), Thrombosis, Dislodgement of previously implanted devices, Tissue damage, Mitral valve stenosis, Persistent or residual mitral regurgitation, Endocarditis; Cardiac arrhythmias (including conduction disorders, atrial arrhythmias, ventricular arrhythmias); Cardiac ischemic conditions (including myocardial infarction, myocardial ischemia, and unstable / stable angina); Venous thromboembolism (including deep vein thrombosis, pulmonary embolism, post procedure pulmonary embolism); Stroke / Cerebrovascular accident (CVA) and Transient Ischemic Attack (TIA); System organ failure: Cardio-respiratory arrest, Worsening heart failure, Pulmonary congestion, Respiratory dysfunction / failure / atelectasis, Renal insufficiency or failure, Shock (including cardiogenic and anaphylactic); Blood cell disorders (including coagulopathy, hemolysis, and Heparin Induced Thrombocytopenia (HIT)); Hypotension / hypertension; Infection including: Urinary Tract Infection (UTI), Pneumonia, Septicemia; Nausea / vomiting; Chest pain; Dyspnea; Edema; Fever or hyperthermia; Pain; Death; Fluoroscopy, Transesophageal echocardiogram (TEE) and Transthoracic echocardiogram (TTE) -related complications: Skin injury or tissue changes due to exposure to ionizing radiation, Esophageal irritation; Esophageal perforation, Gastrointestinal bleeding.
